
Following budget cut, Pembroke revisits future of elementary school re-build
A massive budget cut sustained by the Pembroke School District in March has thrust the future of a long-planned elementary school building project into uncertainty, members of the district’s school board said at a meeting Tuesday.The plan to renovate...

Friends Program completing shelter renovation for families experiencing homelessness
Nancy McKeon hopes that when people think of their time with the Friends Program, where she is the executive director, they’ll remember that they lived in the white house on Thompson Street, rather than a shelter while they were experiencing...
Most Read
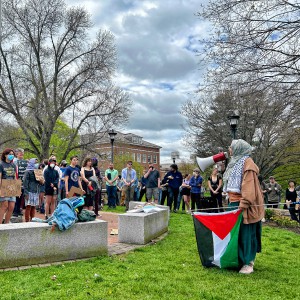 UNH faculty and students call on university police chief to resign following his alleged assault on a student
UNH faculty and students call on university police chief to resign following his alleged assault on a student
 Steeplegate project to reopen to public comment as developer seeks to reduce required parking
Steeplegate project to reopen to public comment as developer seeks to reduce required parking
 Opinion: NH should support SB 553
Opinion: NH should support SB 553
 A turbulent 50-year history: Inside the rise and fall of a tiny Catholic college in Warner
A turbulent 50-year history: Inside the rise and fall of a tiny Catholic college in Warner
 Hopkinton tries to nab out-of-town trash bandits
Hopkinton tries to nab out-of-town trash bandits
 Lawyers and lawmakers assert the Department of Education is on the verge of violating the law
Lawyers and lawmakers assert the Department of Education is on the verge of violating the law
Editors Picks
 A turbulent 50-year history: Inside the rise and fall of a tiny Catholic college in Warner
A turbulent 50-year history: Inside the rise and fall of a tiny Catholic college in Warner
 Hopkinton tries to nab out-of-town trash bandits
Hopkinton tries to nab out-of-town trash bandits
 The murky world of town and city flags in NH
The murky world of town and city flags in NH
 Hopkinton chocolatier transforms chocolates into works of art
Hopkinton chocolatier transforms chocolates into works of art
Sports

High schools: Friday and Saturday results
Girls’ Track Bow 134, Kingswood 24, Pembroke 15 Key players: Bow – Julia Hou (1st 1,600, 1st pole vault, 1st triple jump), Hannah Pawlowski (1st 400, 1st javelin), Camden Wilson (1st high jump, 2nd 100, 2nd 200), Charlotte Weiss (1st discus, 2nd...
 Softball: Cassidy Emerson may have eight freshmen on her team, but the Falcons have glided to an 8-1 start
Softball: Cassidy Emerson may have eight freshmen on her team, but the Falcons have glided to an 8-1 start
 High schools: Hopkinton lax sweeps opponents, more Thursday results
High schools: Hopkinton lax sweeps opponents, more Thursday results
 Celtics turn off Heat; Cavs or Magic on deck
Celtics turn off Heat; Cavs or Magic on deck
 Baseball: Merrimack Valley now 6-1 following wild game at Pembroke Academy
Baseball: Merrimack Valley now 6-1 following wild game at Pembroke Academy
Opinion
Opinion: The slippery slope that should scare us? The trend of legislatures getting involved in personal medical decisions.
Cappy and Mark Nunlist live in Lebanon. HB 1283, the Medical Aid in Dying Bill (MAiD), has passed the NH House by a slim margin and is now before the Senate. The three primary objections to the bill are one, the bill will morph into a mandate to...
 Opinion: Thank goodness for New Hampshire teachers
Opinion: Thank goodness for New Hampshire teachers
 Opinion: NH should support SB 553
Opinion: NH should support SB 553
 Opinion: Let’s not go back
Opinion: Let’s not go back
 Opinion: The inspiring life of Howard Zinn
Opinion: The inspiring life of Howard Zinn

Politics

House passes bill to raise minimum marriage age to 18, sending it to governor
The New Hampshire House passed a bill Thursday raising the legal age of marriage to 18, sending the legislation to Gov. Chris Sununu’s desk after years of advocacy.Senate Bill 359, which passed 192-174, states that “no person below the age of 18 years...
 Charities will not have to pay rent to casinos under new law
Charities will not have to pay rent to casinos under new law
 Sununu says he’ll support Trump even if he’s convicted
Sununu says he’ll support Trump even if he’s convicted
 NH mayors want more help from state on homelessness prevention funds
NH mayors want more help from state on homelessness prevention funds
 Two democrats with parallel views run for same State Senate seat
Two democrats with parallel views run for same State Senate seat
Arts & Life

Northeast Coffee Festival comes to Concord this weekend
Coffee and tea amateurs and professionals will flock to downtown Concord on May 10 and 11 to experience the Northeast Coffee Festival. The free outside portion of the event will include two full days of live music and over 30 local vendors. Coffee and...
 Henniker Handmade & Homegrown
Henniker Handmade & Homegrown
 Colonial Theatre Laconia presents Piff the Magic Dragon
Colonial Theatre Laconia presents Piff the Magic Dragon
 The Loft at Hermit Woods presents Pete Kilpatrick
The Loft at Hermit Woods presents Pete Kilpatrick
 24th Annual Perennial Exchange opens Concord’s gardening season
24th Annual Perennial Exchange opens Concord’s gardening season
Obituaries
 Miriam Chamberlin
Miriam Chamberlin
Concord, NH - Miriam Helen (Gaskell) Chamberlin, 92, passed away Saturday April 20, 2024 at Pleasant View Center nursing home, Concord, NH, after a long period of failing health. She was born in Concord, NH on February 25, 1932, the dau... remainder of obit for Miriam Chamberlin
 Junie Landry
Junie Landry
Mesa, AZ - Junie L. Landry, 93, passed away after a sudden illness on Tuesday, April 9, 2024. She was born in May, 1930 in Laconia, NH, to Harry S. and Thelma I. (Trumbull) Waite. She attended Laconia High School while living at 56... remainder of obit for Junie Landry
 Sandra Scheys
Sandra Scheys
Bow, NH - Sandra Renee Scheys, age 60, died on Tuesday, April 16th, 2024 at St. Vincent's Hospital in Worcester, MA, after a short battle with cancer. Born on July 22, 1963 in Concord, Sandie attended schools in Bow, NH and Bishop B... remainder of obit for Sandra Scheys
 Joseph M. Jenovese Jr.
Joseph M. Jenovese Jr.
Concord, NH - Joseph M. Jenovese Jr., age 88, of Eastside Drive, Concord, passed away peacefully at his home on Sunday, April, 28th 2024, surrounded by his family, following a period of declining health. He was born on November 11th, 19... remainder of obit for Joseph M. Jenovese Jr.

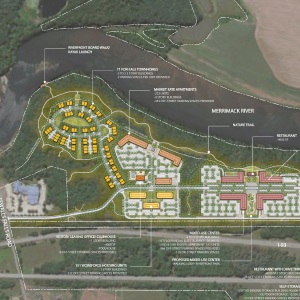 Monitor Way developer seeks $4.67 million from city for proposed new road
Monitor Way developer seeks $4.67 million from city for proposed new road
 Transgender sports ban receives Senate committee support
Transgender sports ban receives Senate committee support
 NH Senate panel frowns on bill to ease vehicle inspection requirements
NH Senate panel frowns on bill to ease vehicle inspection requirements
 Expanded degree offerings at KSC, Plymouth State among panel's recommendations
Expanded degree offerings at KSC, Plymouth State among panel's recommendations
 In New Hampshire governor’s race, some finance reports are clearer than others
In New Hampshire governor’s race, some finance reports are clearer than others
 Opinion: Protecting NH from PFAS
Opinion: Protecting NH from PFAS
 Boys’ lacrosse: Through the lumps, Concord coach thinks young team is ahead of schedule
Boys’ lacrosse: Through the lumps, Concord coach thinks young team is ahead of schedule
 High schools: Monday’s baseball, softball, lacrosse and tennis results
High schools: Monday’s baseball, softball, lacrosse and tennis results


